Starting a course of biologic therapies is a huge step toward managing chronic conditions like rheumatoid arthritis or Crohn's disease. But for many, the transition to self-injection feels like being thrown into the deep end of a pool without knowing how to swim. While these large-molecule drugs are life-changing, the way you put them into your body matters just as much as the drug itself. If your training was a quick five-minute chat in a busy clinic, you aren't alone-and you might be at a higher risk for complications than you realize.
The Gap Between Training and Reality
Most people assume that if a doctor gives them a prescription for a biologic, they'll get a full masterclass on how to use it. In reality, there's a massive gap. Research shows that while over 90% of patients say they received training, it usually lasts only about 30 minutes. Compare that to the 90 to 120 minutes experts say is actually needed to feel confident, and it's easy to see why so many people struggle.
Think about it: you're dealing with a powerful medication, a needle, and often a lot of anxiety. When training is rushed, patients often miss the "try/do" phase-the part where you actually handle the device under supervision. Without this, the first few injections at home become a guessing game. In fact, nearly 70% of technique errors happen during the first ten home injections because the clinical setting doesn't prepare you for the distractions and nerves of your own living room.
Understanding the "Tell, Show, Do" Framework
To really nail the technique, training shouldn't just be a conversation. It needs to follow a three-step process. If you're missing any of these, it's worth asking your provider for a follow-up session.
- Tell: This is the verbal instruction. Your nurse explains where to inject and how the device works.
- Show: The provider demonstrates the process using a training device or the actual medication.
- Do: This is the gold standard. You use a training device-a needle-less replica of the pen-to practice the grip, the click, and the timing until it feels like second nature.
Interestingly, a "teach-back" method is way more effective than just listening. This is where you explain the process back to the nurse or demonstrate the step. It’s over three times more effective at ensuring you don't make a mistake once you're home alone.
The Real Risks: Infection and Sterile Fields
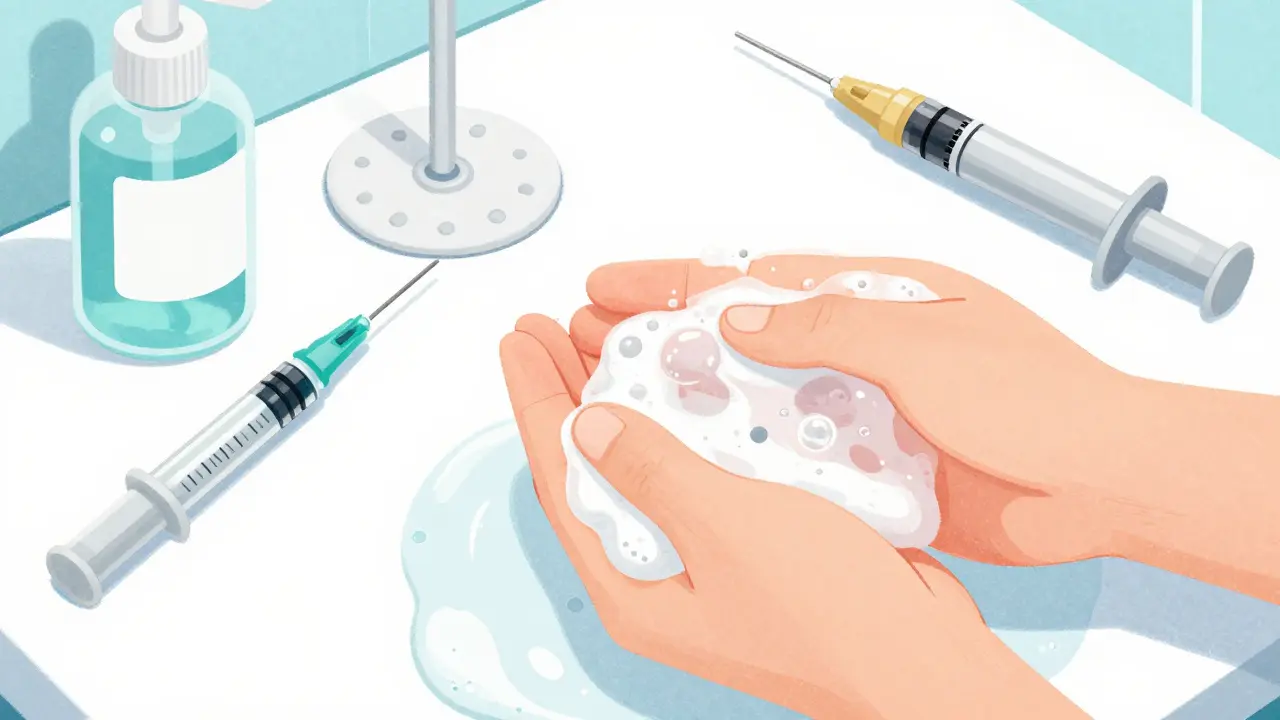
This is where the stakes get high. A biologic injection isn't like a quick flu shot; it's a recurring process that requires a strict sterile field. According to the CDC, poor injection technique can spike your infection risk by 37%. Most of these infections aren't caused by the drug itself, but by bacteria being pushed into the skin because of a compromised environment.
Common pitfalls include skipping the 20-second soap-and-water hand wash or failing to properly clean the injection site. Some patients mistake a localized skin reaction for an infection, but a real infection is a serious matter. You should be on high alert if you notice redness that spreads beyond 2 centimeters in diameter or if you develop a fever over 100.4°F (38°C). These are red flags that require immediate medical attention.
| Training Model | Approach | Patient Outcome | Retention Rate |
|---|---|---|---|
| Single-Session | One-time clinic demo | Higher initial anxiety | Lower (approx. 52%) |
| Distributed | Multiple short sessions | Higher confidence | High (62% increase) |
| Just-in-Time | Digital guides used during act | Fewer technique errors | 48% error reduction |
Mastering the Mechanics: A Safety Checklist
To minimize the risk of infection and ensure the medication is absorbed correctly, you need a repeatable system. Experts suggest creating an "injection ritual"-a set sequence of events that anchors the process and lowers anxiety.
- Prep your space: Clear a hard, flat surface. Ensure you have good lighting so you can see exactly where the needle is going.
- Hand Hygiene: Scrub your hands for 20 seconds. This is the simplest way to prevent skin and soft tissue infections.
- Site Selection: Rotate your sites to avoid skin thickening. Use the thigh, abdomen (avoiding the belly button), or upper arm. Keep at least a 1-inch gap between your last injection and the new one.
- The "Breathing Room" Trick: If you're nervous, imagine a provider's hand over yours, guiding you to hold the device firmly against the skin. Don't pull the needle out too early; wait for the device to signal the dose is complete.
- Safe Disposal: Never throw needles in the regular trash. Use a puncture-proof sharps container to prevent accidental injuries to yourself or sanitation workers.

Addressing the Emotional Hurdle
We often treat injection training like a math problem-just follow the steps and you'll get the right answer. But for many, the fear of needles (trypanophobia) or the stress of a chronic diagnosis creates a mental block. This emotional weight is responsible for over half of the patients who quit their therapy in the first year, even if they know exactly how the pen works.
Building a routine helps. Whether it's putting on a specific playlist or having a rewarding snack afterward, these rituals turn a scary medical task into a manageable habit. If you're feeling overwhelmed, don't hesitate to lean on your pharmacist. Pharmacists are often underutilized resources who can provide the detailed counseling and technique checks that a rushed doctor's visit might miss.
Looking Ahead: The Future of Self-Administration
The industry is finally catching up. We're seeing a shift toward digital training portals with video coaching and virtual trackers. The FDA has also begun emphasizing the need for structured, consistent resources rather than leaving training up to the individual clinic's discretion. As we move toward 2027, the goal is to blend mechanical skill with emotional support, ensuring that the therapy actually reaches the patient safely and effectively.
How do I know if my injection site is infected or just reacting to the drug?
It's common to see some mild redness or a small bump after a biologic injection. However, if the redness expands beyond 2cm, feels hot to the touch, or is accompanied by a fever of 100.4°F (38°C) or higher, it could be an infection. Contact your healthcare provider immediately if these symptoms occur.
Can I use a training device if I've already started my medication?
Yes. In fact, continuing to use a trainer device can help maintain your confidence and technique, especially if you take a break from therapy or switch to a different brand of biologic pen.
Why is site rotation so important?
Injecting the same spot repeatedly can cause lipohypertrophy (thickening of the skin and fat), which can interfere with how the medication is absorbed into your bloodstream. Always leave at least one inch of space from your previous injection site.
What should I do if I feel too anxious to inject myself?
Start by using a training device to desensitize yourself to the mechanism. Try establishing a "ritual" (like a specific set of calming actions) before the injection. If anxiety persists, ask your doctor for a supervised session where they can use the "breathing room" technique to guide your hand.
How long should I wash my hands before an injection?
The CDC recommends scrubbing your hands with soap and water for at least 20 seconds. This significantly reduces the risk of introducing bacteria into the injection site, which is a primary cause of outpatient skin infections.


Tama Weinman
19 Apr 2026 at 17:43Funny how the 'experts' only want you to spend 30 minutes on training. It's almost like they want us dependent on their expensive 'follow-up' sessions. Just follow the money trail and you'll see why the system is designed to keep you anxious and shaky. Maybe if we actually looked at the patents for these delivery devices, we'd realize they're designed for planned obsolescence of the patient's confidence. Typical corporate medical industrial complex nonsense.