Imagine your stomach has a built-in shield-a thick layer of mucus that stops powerful digestive acids from eating through your own organs. When this shield breaks down or gets irritated, you end up with gastritis is an inflammation of the protective lining in the stomach (the mucosa). It isn't just a simple "upset stomach"; it can range from a sudden, sharp attack to a slow-burning irritation that lasts for years. If left alone, it can lead to ulcers or even more serious complications. The good news? Most cases are completely treatable once you identify whether the cause is a stubborn bacteria, a lifestyle habit, or a reaction to medication.
What Exactly Is Happening to Your Stomach?
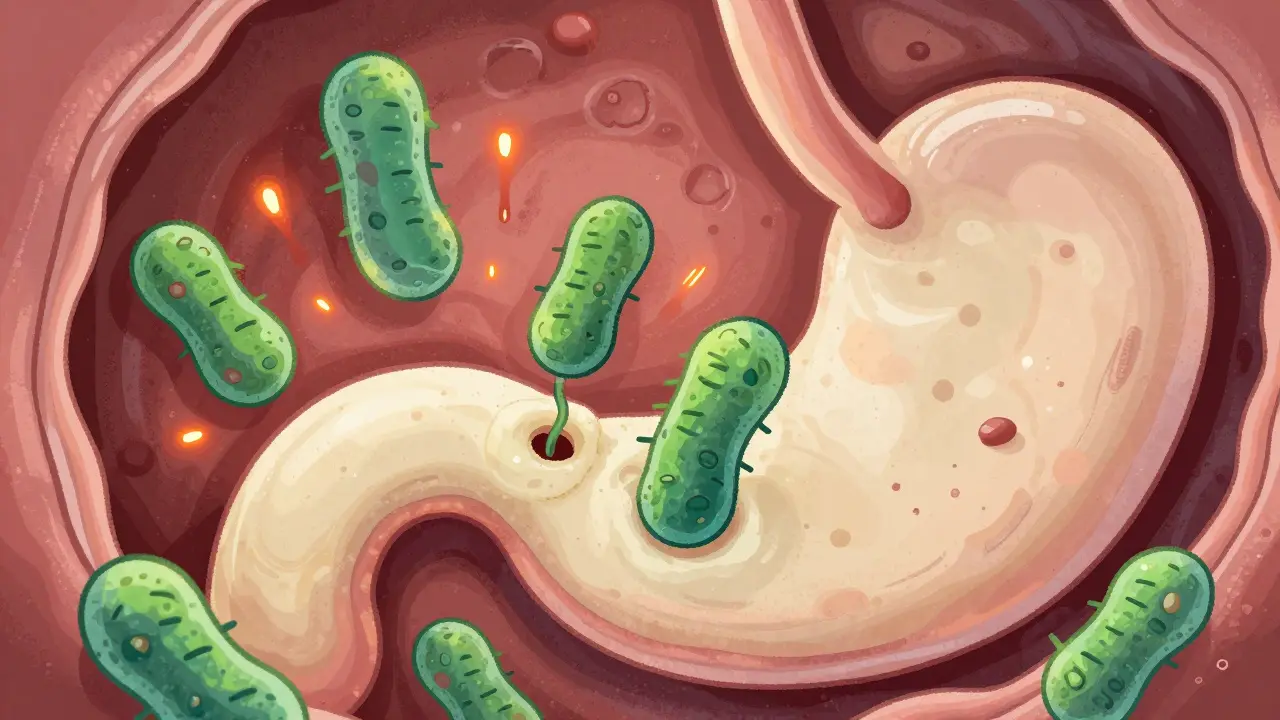
To understand gastritis, you have to look at the stomach wall. Your stomach produces acid to break down food, but it also produces a mucus barrier to protect itself. When that barrier is compromised, the acid leaks into the stomach wall, causing inflammation. Doctors generally split this into two main types: erosive and nonerosive.
Erosive gastritis is the more "aggressive" version. It involves actual physical breaks or wear-and-tear in the lining. This is often what happens when people take too many painkillers like NSAIDs (Non-Steroidal Anti-Inflammatory Drugs) such as ibuprofen or aspirin. On the other hand, nonerosive gastritis is more subtle. There are no visible holes, but the cells are changing. One common version is atrophic gastritis, where the lining thins out and the stomach loses its ability to produce the acid it needs for digestion.
The H. pylori Connection: The Most Common Culprit
For a long time, doctors weren't sure why some people got chronic stomach inflammation. That changed when researchers discovered Helicobacter pylori (or H. pylori) is a spiral-shaped bacterium that infects the stomach lining and survives the acidic environment. This tiny bug is responsible for a massive amount of the world's gastritis cases-roughly 70-90% of gastric ulcers are linked back to this specific infection.
H. pylori doesn't just sit there; it actively weakens the protective mucus layer, allowing acid to seep in. In some people, it causes almost no symptoms for decades. In others, it leads to a cycle of nausea and burning pain. Because it's so common (affecting hundreds of millions globally), knowing how to spot it and kill it is the cornerstone of gastrointestinal health.
| Feature | Acute Gastritis | Chronic Gastritis |
|---|---|---|
| Onset | Sudden, rapid | Gradual, insidious |
| Primary Causes | Alcohol, NSAIDs, severe stress | H. pylori, autoimmune reactions |
| Key Symptoms | Sharp pain, vomiting, nausea | Bloating, mild discomfort, anemia |
| Typical Goal | Immediate symptom relief | Eradication of bacteria/long-term monitoring |
Spotting the Warning Signs
Most people with acute gastritis feel it immediately: a gnawing or burning ache in the upper abdomen, nausea, and sometimes vomiting. However, chronic gastritis is a sneakier beast. Up to half of the people with chronic inflammation don't even know they have it until it turns into something worse.
You need to pay attention to "red flag" symptoms. If you notice black, tarry stools (melena) or if you vomit something that looks like coffee grounds, stop reading and call a doctor. These are classic signs of internal bleeding. Other warning signs include unexplained fatigue or shortness of breath, which often point to anemia because your stomach is losing blood or failing to absorb nutrients properly.
How Doctors Diagnose the Problem
You can't diagnose gastritis with a blood test alone. The "gold standard" is an Endoscopy, where a doctor slides a small camera down your throat to look at the stomach lining and take a tiny piece of tissue (a biopsy) for testing. This is the only way to be 100% sure about the type of inflammation and whether H. pylori is present.
If you're looking for a less invasive route, the urea breath test is incredibly accurate. You drink a special solution and breathe into a bag; if the bacteria are present, they break down the solution and release a specific gas that the test detects. It has a success rate of over 90% for spotting H. pylori without needing to put a camera in your stomach.
Tackling H. pylori and Healing the Lining
If the tests come back positive for H. pylori, the goal is simple: kill the bacteria and stop the acid. The standard approach is "triple therapy," which usually involves a Proton Pump Inhibitor (PPI) (like omeprazole) and two different antibiotics. The PPI shuts down the acid production, which makes the environment less hospitable for the bacteria and gives the lining a chance to heal, while the antibiotics do the heavy lifting of killing the infection.
But there's a catch: antibiotic resistance. In some regions, the bacteria have learned to survive common drugs like clarithromycin. If the first round of treatment fails, doctors might switch to bismuth quadruple therapy or newer drugs like vonoprazan, which blocks acid more effectively than traditional PPIs. A critical mistake many people make is stopping their antibiotics early because they "feel better." Doing this often allows the strongest bacteria to survive, leading to a much harder-to-treat second infection.

Lifestyle Shifts for Lasting Recovery
Medication handles the fire, but lifestyle changes prevent it from starting again. If your gastritis is caused by alcohol or smoking, the results of quitting are almost immediate. Stopping alcohol can reduce symptom severity by 60% in as little as two weeks. Similarly, if you rely heavily on ibuprofen or aspirin for joint pain, switching to a stomach-friendly alternative (after consulting your doctor) can stop the erosive cycle.
For those with rare autoimmune gastritis, the challenge is different. Your body attacks the cells that produce "intrinsic factor," which is necessary to absorb vitamin B12. In these cases, no amount of diet change will fix the problem-you'll need lifelong B12 injections to prevent nerve damage and severe anemia.
How long does it take for gastritis to heal?
Acute symptoms usually improve within 7 to 10 days with the right medication. However, if you have H. pylori, the eradication treatment takes 10 to 14 days of antibiotics, and full healing of the stomach lining can take several weeks of acid suppression. A follow-up breath test is usually done 4 weeks after treatment to confirm the bacteria are gone.
Can I cure gastritis with diet alone?
Diet can manage symptoms and support healing, but it cannot cure an H. pylori infection. Antibiotics are required to remove the bacteria. Avoiding triggers like spicy foods, alcohol, and caffeine can reduce irritation, but treating the underlying cause (like the bacteria or NSAID use) is the only way to achieve a permanent cure.
What are the risks of taking PPIs for too long?
While PPIs are great for short-term healing, long-term use can lead to a "rebound effect" where the stomach produces even more acid once you stop the drug. Some evidence also suggests that prolonged use may interfere with the absorption of magnesium and B12, which is why doctors prefer using them for the shortest time necessary.
Is H. pylori contagious?
Yes, H. pylori is believed to spread through saliva or fecal-oral contact. While the exact mechanism isn't fully understood, it's common in households and areas with poor sanitation. This is why in some families, multiple members may test positive for the infection.
What is the difference between a stomach ulcer and gastritis?
Gastritis is the general inflammation of the stomach lining. An ulcer is a deeper, specific hole or sore that has worn through that lining. You can think of gastritis as a widespread "rash" inside the stomach, while an ulcer is a localized "crater." Often, untreated gastritis leads to the formation of ulcers.
Next Steps: What Now?
If you're currently dealing with stomach pain, your first move should be a diary. Note what you eat, which medications you take, and when the pain hits. This helps your doctor decide if they need to jump straight to an endoscopy or start with a non-invasive breath test. If you are prescribed a 14-day course of antibiotics, set alarms on your phone-missing just a few doses can lead to treatment failure and antibiotic resistance.
For those who have already finished treatment, don't assume you're in the clear just because the pain stopped. Make sure to get that 4-week follow-up test. Confirming the bacteria are actually dead is the only way to ensure you've lowered your long-term risk of gastric complications.




Victor Parker
10 Apr 2026 at 23:16Big Pharma just wants you on those PPIs forever 🙄 They don't tell you that the 'bacteria' is just a cover for the toxins they put in the water supply anyway 👁️ Keep your eyes open folks!